Diabetic Foot Ulcer and Platelet-Rich Plasma
Dear Readers,
First and foremost, my advanced apologies for the long absence since Christmas. The season to be jolly truly turned out to be one with never ending things to do for both family, friends and patients included.
So here goes my first topic for the new year – 2015.
We all know that Diabetes Mellitus is a pandemic that has plagued mankind for centuries now. The disease is centered on dysfunctional glucose regulation and metabolism – leading to a state of persistent hyperglycemia. This results in corrosion of small and large blood vessels alike. Following years of persistent corrosion, Diabetes causes target organ damage especially of the kidneys, retina and micro capillaries. Diabetic Foot Ulcers (DFU) occur when vascular perfusion to the foot and toe digits are compromised causing persistent tissue ischaemia – meaning low oxygenation. We all know that our cells mandatorily require oxygen to survive, grow and replicate. So what happens when oxygen becomes a scarcity to the tissues of the foot, which is also routinely exposed to the environment and our daily weight bearing? The skin and tissues have now become very vulnerable and the slightest of trauma may provoke a detrimental cascade of events that can even result in an amputation. A recent study states that Diabetes causes 1 million amputations a year.
But before I go there, I would like to highlight some salient points and the general treatment of a DFU.
1. Never walk barefoot. The nerve damage decreases sensation so you may not notice small abrasions or trauma. Always wear shoes or slippers to reduce this risk.
2. Wash your feet every day with mild soap and warm water. Do not soak your feet. Pat dry with a towel. Be gentle.
3. Use lotion to keep the skin of your feet soft and moist. This prevents dry skin cracks and decreases the risk of infection. Do not put lotion between the toes.
5. Do not use antiseptic solutions, drugstore medications, heating pads, or sharp instruments on your feet.
6. Always keep your feet warm. Wear loose socks to bed.
7. Do NOT smoke. Smoking damages blood vessels and decreases the ability of the body to deliver oxygen. In combination with diabetes, it significantly increases your risk of amputation — not only of the feet, but can include the hands, as well.
Definitive treatment includes regular and appropriate wound dressings and debridements by your doctor.
So now coming to the interesting bit. where does PRP come in all this. Please forgive my enthusiasm, simply because I have recently treated one such DFU with PRP, and the results were absolutely great. It started off as a trial to which patient had consented, but after four weeks of PRP and follow ups – the outcome was quite astounding. Unfortunately the pictures of the concerned patient cannot be uploaded, but instead I will take you through her progress in a more literary manner.
Before that, an overview of PRP – Platelet Rich Plasma:
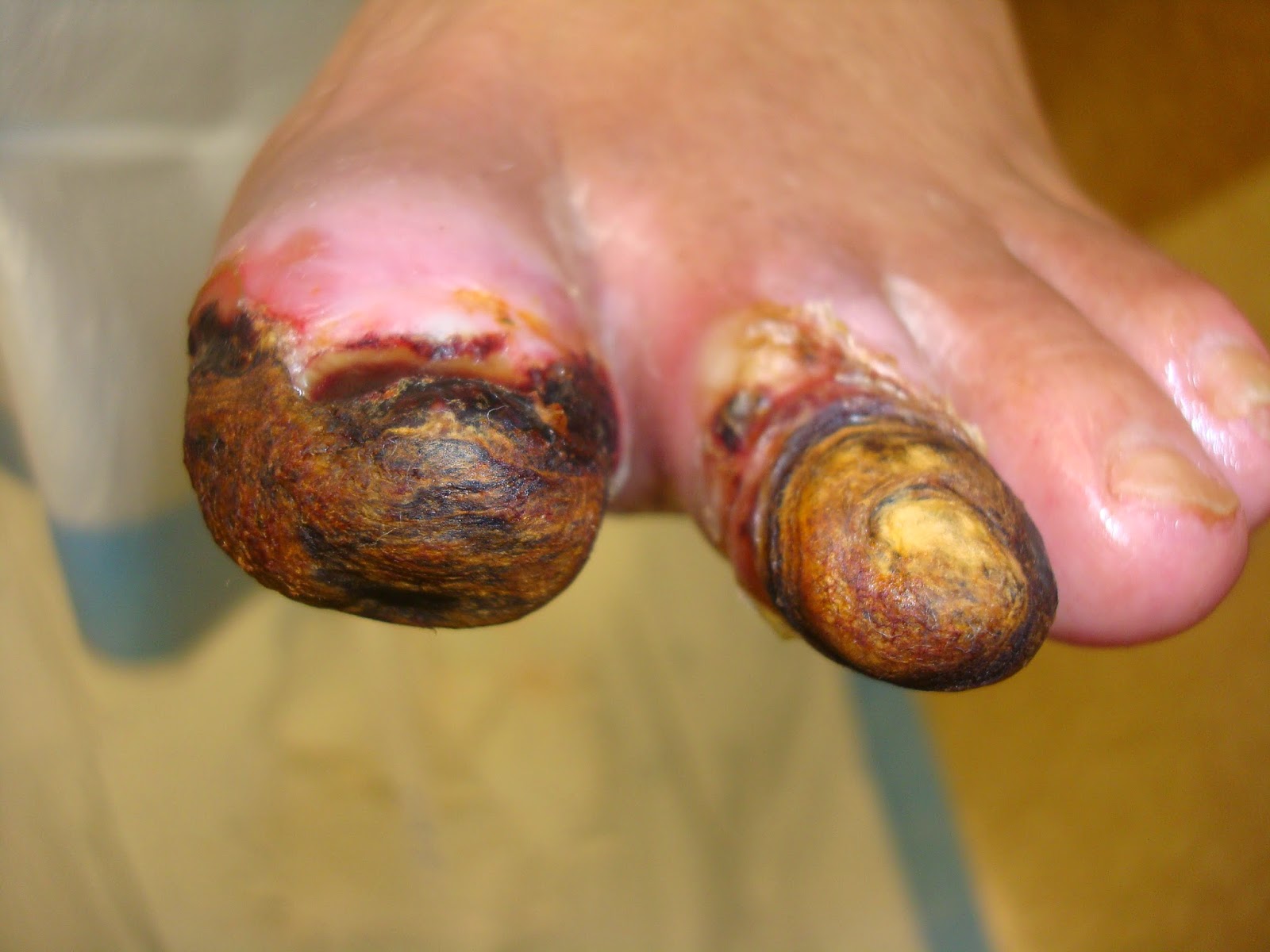
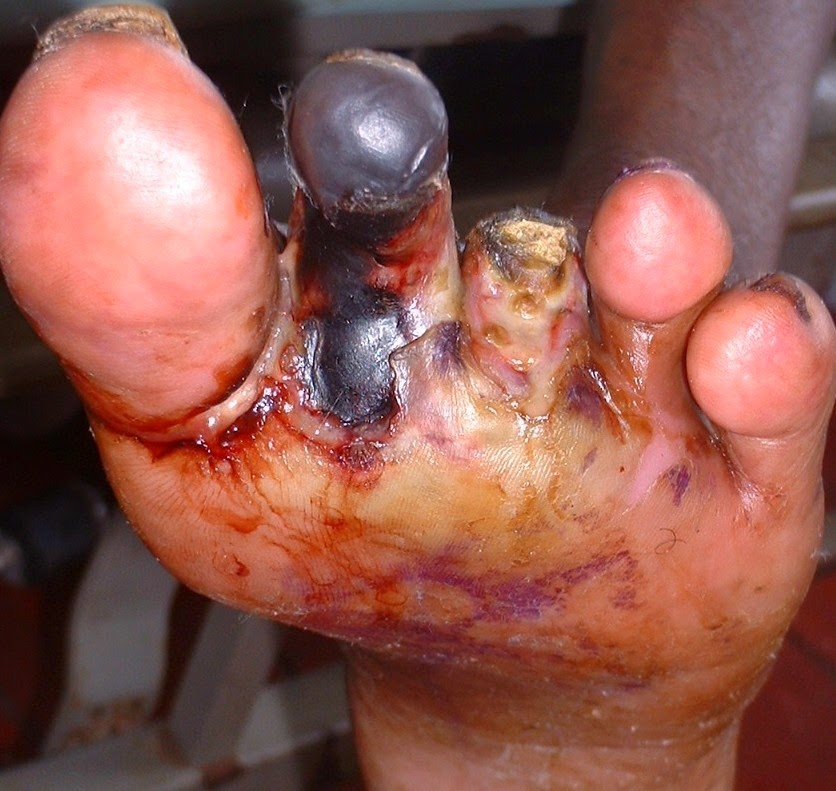
My patient had a typical DFU with areas of dry gangrene and almost 80% loss of soft tissues in one of her toes. The tendons and bones were visible, and the entire wound was infected with pus and foul smelling discharge. The front of her foot was darkened with hyperpigmentation and the skin was dry and cracked. She was also suffering from a lot of pain. She was extremely anxious that there would be no choice except for an amputation of the digit.
It was at this junction, that I suggested the PRP treatments for her. It took me some time to explain to her how the treatment would be conducted and how it would benefit her. She agreed and I silently hoped I could help provide her the result she wanted.
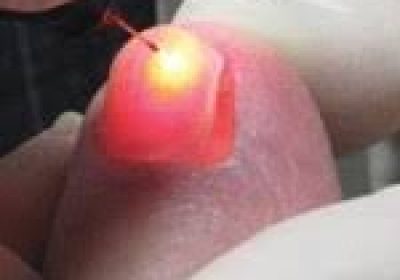
Treatment included direct injection of autologous PRP into the toe digits and skin of the foot, after complete cleansing and debridement. Approximately 3ml of PRP was injected each time and another 3ml of PRP was applied topically on to the wound. Dressing composed of PRP soaked gauze and topical antibiotics. This was repeated weekly for a month.
In her last review, the improvement was short of excellent. The tendons and tarsal bones were no longer visible, as healthy granulation tissue had grown to fill up the previously empty digital skeleton. The skin of the foot was less pigmented and lichenified. The patient also felt the mobility and comfort level of her foot had improved.
So what actually had transpired?
The platelets in the PRP act as healing agents that help to mend the wound via aggregation and cellular cohesion. The abundant growth factors inside the plasma generate new vessels – a process called angiogenesis, stimulate cellular growth and differentiation. The new vessels increase cellular oxygenation and assist in deterring infections by creating an aerobic environment. The end result is tissue and neurovascular genesis within the affected toe.
I would like to conclude that PRP is definitely an alternative and effective treatment modality when conventional medicine fails to provide adequate improvement. It has numerous other indications including scar revision, facial rejuvenation, venous, arterial & pressure ulcers, superficial thermal wounds, vitiligo, skin graft sites, hair loss, sports injury and cutaneous & musculoskeletal degeneration.
For more information on PRP, do make an appointment with myself at Premier Clinics, Bangsar or TTDI branch.
Thank You.